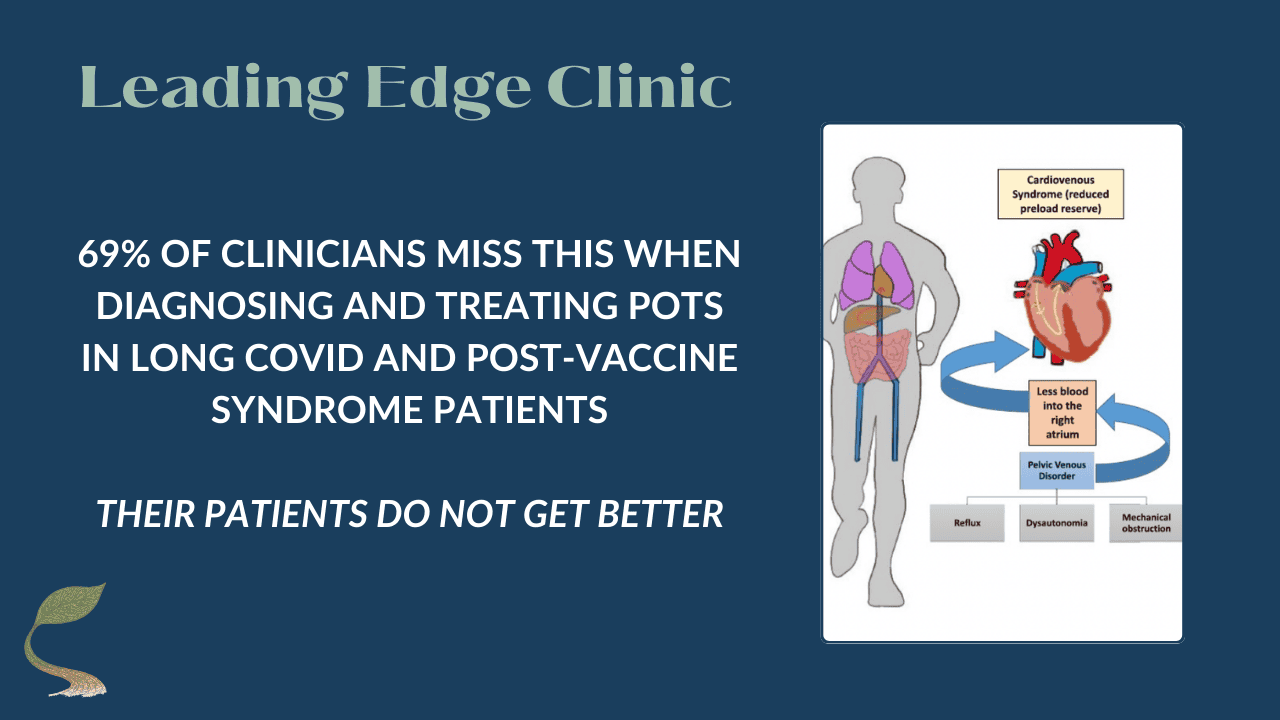
If you developed POTS (Postural Orthostatic Tachycardia Syndrome) after COVID infection or vaccination, you’ve probably been told to:
- Drink more water and increase salt
- Wear compression stockings
- Try beta-blockers or midodrine
- Do gradual exercise reconditioning
And maybe you’ve tried all of these. Some helped a little. But you’re still dealing with:
- Racing heart when you stand up
- Dizziness and lightheadedness
- Extreme fatigue after being upright
- Brain fog that worsens throughout the day
- Feeling like you’re going to pass out
- Significant symptom burden first thing in the morning
Here’s what we’ve learned after treating thousands of Long COVID and Post-Vaccine Syndrome patients with POTS:
Standard POTS treatments address the symptoms. But in 70% or more of the patients who come to us, there’s an underlying structural problem that’s driving the whole thing. A problem that most doctors don’t know to check for.
And when we fix this underlying problem? Many patients see dramatic improvement, sometimes within days of treatment.
The Hidden Problem Most Doctors Miss
After treating patients with post-viral and post-vaccine POTS since 2020, we’ve found something striking:
Over 70% of our POTS patients have significant venous compression in their pelvis.
Specifically, compression of the left common iliac vein, which is the major vein that drains blood from your left leg back to your heart.
This isn’t some fringe condition. Research shows:
- 69% of POTS patients have significant iliac vein compression (compared to 40% of healthy controls)
- Up to 80% of POTS patients have some form of pelvic venous insufficiency
- Yet most doctors never evaluate for it
Why does this matter?
Because if your POTS is being driven by poor venous return to your heart, all the salt and compression stockings in the world won’t fix the underlying problem.
It’s like trying to fill a bucket that has a hole in the bottom. You can keep pouring water (blood volume expansion, medications), but if the drainage system is blocked, you’re not solving the actual issue.
What Is Iliac Venous Compression?
Your left common iliac vein sits behind your right common iliac artery. In the normal anatomy, this is fine. Blood flows through both vessels without issue.
But in many people, especially after spike protein exposure from COVID or vaccination, the vein gets compressed by the artery sitting on top of it.
This compression is called May-Thurner Syndrome or iliac venous compression syndrome.
What happens when this vein is compressed?
- Blood from your left leg can’t return to your heart efficiently
- Blood pools in your lower body, worsened by postural changes such as standing
- Less blood returns to your heart
- Your heart has to beat faster to maintain blood pressure (hello, POTS)
- You get all the classic POTS symptoms
Here’s the key insight: While this is an anatomical quirk that some people are born with, there still needs to be an activating event.
In Long COVID and Post-Vaccine Syndrome patients, spike protein is actively causing this problem through two main pathologies that impact the structural integrity of blood vessel walls.
—
Clinical Observation from Leading Edge Clinic:
In our practice, we’ve observed that many Long COVID and Post-Vaccine Syndrome patients present with venous compression that wouldn’t have been clinically significant before spike protein exposure. The spike-induced endothelial and collagen dysfunction appears to transform anatomical variations that were previously asymptomatic into symptomatic compression syndromes.
One representative case: A 34-year-old female developed severe POTS 6 months post-vaccination. Imaging revealed 60% left common iliac vein compression—a finding that may have been present anatomically for years but only became symptomatic after spike protein triggered endothelial dysfunction and reduced her venous compliance.
Another case: A 30 year old male had a gradual onset of POTS that eventually became severe post-vaccination. Prior to Post-Vaccine Syndrome, patient was active, working out 6 days a week (hot yoga, kettlebell HIIT workouts, 30 mile cycling rides, etc…). A 3 day treatment of stem-cell exosomes improved some chest pain symptoms, but the POTS symptoms remained. Patient found mornings to be particularly difficult, with leg pain upon waking. Minor exertion caused continued chest pain and poor recovery. MRA and MRV revealed a significant stenosis indictative of IVC, which was confirmed by Dr. Brooke Spencer during an IVUS at stenting procedure. The IVUS showed an 80+% stenosis. POTS symptoms resolved upon stenting.
From the clinical observations of Dr. Scott Marsland, practice partner at Leading Edge Clinic
—
The Spike Protein Connection
Why do so many Long COVID and Post-Vaccine Syndrome patients develop venous compression?
Two mechanisms:
1. Endothelial Dysfunction
Spike protein damages the endothelium (the inner lining of blood vessels), especially the glycocalyx. This causes:
- Inflammation of vessel walls
- Reduced elasticity
- Impaired vascular function
- Makes veins more susceptible to compression
Your veins rely on healthy endothelium to maintain their structure and resist external pressure. When spike protein damages this lining, the veins become weaker and more easily compressed.
2. Collagen Dysfunction
Spike protein also interferes with normal collagen synthesis and function. This creates a situation similar to what we see in Ehlers-Danlos Syndrome (EDS):
- Weakened connective tissue
- Reduced structural support for veins
- Increased vein distensibility (they stretch and collapse more easily)
- Higher risk of venous compression syndromes
Think about it like this: If the walls of your vein are weakened by spike-induced collagen dysfunction, they’re more likely to collapse under the pressure of the artery sitting on top.
This is why we see such high rates of venous compression in Long COVID and Post-Vaccine Syndrome patients compared to the general population. Before spike protein was in our environment, symptomatic iliac venous compression was triggered by acute traumatic events, such as childbirth in women. Or, in chronic conditions that are less prevalent, less virulent, than Long Covid and Post-Vaccine Syndrome (ie: Lymes disease).
What We’re Seeing in Practice
After evaluating hundreds of Long COVID and Post-Vaccine Syndrome patients with POTS, we’ve identified consistent patterns:
Collagen dysfunction markers:
- Patients who previously had no hypermobility now showing joint laxity
- Skin changes consistent with collagen degradation
- Venous fragility (easy bruising, visible spider veins developing post-illness)
- These changes correlate with severity of venous compression
Endothelial dysfunction markers:
- Persistent microclots under flurosescence microscope
- Elevated inflammatory markers (IL-6, IL-8)
- Visible microvascular changes (reticular veins, telangiectasias)
- Poor vascular reactivity
The pattern we see: Patients with more severe endothelial and collagen dysfunction tend to have worse venous compression, even with similar anatomical compression ratios.
This suggests spike protein damage intensity determines symptom severity more than degree of anatomical compression alone.
How This Causes POTS: The Vicious Cycle
Here’s how iliac venous compression drives POTS symptoms:
Standing up triggers a cascade:
- Gravity pulls blood down to your legs
- Your compressed iliac vein can’t efficiently return blood to your heart
- Blood pools in your lower body (venous pooling)
- Cardiac output drops (less blood returning = less blood pumping out)
- Baroreceptors sense the drop in blood flow
- Your nervous system kicks into overdrive to compensate
- Heart rate shoots up to try to maintain blood pressure
- You feel terrible: dizzy, lightheaded, tachycardic, exhausted
Meanwhile, the pooled blood isn’t delivering oxygen efficiently to your brain and tissues.
This explains why POTS patients often have:
- Severe brain fog (reduced cerebral blood flow)
- Extreme fatigue (poor oxygen delivery to tissues)
- Exercise intolerance (can’t increase cardiac output effectively)
- Worsening symptoms as the day progresses (cumulative venous pooling)
The Hidden Connection: How Venous Compression Triggers MCAS
If you have both POTS and MCAS (Mast Cell Activation Syndrome), you might have noticed they seem to feed into each other. You’re not imagining it.
There’s a connection most doctors miss:
Venous compression doesn’t just cause POTS symptoms. It actively worsens mast cell activation.
How Venous Congestion Triggers Mast Cells
When blood pools in your lower body due to venous compression:
1. Tissue hypoxia (low oxygen)
- Pooled blood isn’t circulating properly
- Tissues become oxygen-deprived
- Hypoxia is a potent mast cell degranulation trigger
2. Inflammatory mediator accumulation
- Normal venous drainage clears inflammatory substances
- Compressed veins can’t drain efficiently
- Histamine, prostaglandins, and other mediators accumulate
- Creates a high-histamine environment in tissues
3. Endothelial stress
- Venous hypertension (increased pressure from poor drainage)
- Stressed endothelium releases inflammatory signals
- Mast cells respond by degranulating
4. The POTS-MCAS Spiral
- Venous compression → POTS symptoms (tachycardia, poor perfusion)
- POTS symptoms → stress response, poor tissue perfusion
- Stress and hypoxia → mast cell activation
- Mast cell mediators → more inflammation, more vascular dysfunction
- Worse vascular function → more venous compression
- Round and round it goes
Why This Matters for Treatment
If you treat MCAS but ignore venous compression:
- Antihistamines and mast cell stabilizers help temporarily
- But the underlying trigger (venous congestion) persists
- MCAS keeps flaring despite medication
- “I’m on 6 different MCAS medications and still symptomatic”
If you treat venous compression:
- Improved venous drainage reduces tissue hypoxia
- Better circulation clears inflammatory mediators
- Less mast cell triggering
- MCAS symptoms often improve significantly
- Some patients need fewer MCAS medications
This is why so many patients have the “POTS-MCAS-EDS trifecta.” The mechanisms overlap and reinforce each other. Treating venous compression addresses a root cause that’s driving both conditions.
Why Standard POTS Treatments Don’t Work for Venous Compression
Let’s look at why the usual approaches fall short when venous compression is the underlying issue:
Salt and Hydration
Standard advice: Increase salt and fluid intake to expand blood volume.
Why it doesn’t fully work: You’re expanding the volume, but the venous “highway” is still blocked. The blood still can’t get back to your heart efficiently. You might get minor improvement, but you’re not addressing the structural obstruction.
Our experience: Patients often say “I’m drinking so much water and salt I feel bloated, but I’m still symptomatic.”
Compression Stockings
Standard advice: Wear compression stockings to reduce venous pooling in the legs.
Why it doesn’t fully work: Compression stockings help prevent blood from pooling in the lower leg veins. But if the iliac vein is compressed, blood still can’t get past that obstruction to reach the heart. You’re compressing the bottom of the system while the top is blocked.
Our experience: “The stockings help a little, but I still crash after standing for 15 minutes.”
Beta-Blockers and Midodrine
Standard advice: Beta-blockers to slow heart rate, midodrine to constrict blood vessels and raise blood pressure.
Why it doesn’t fully work: These are symptomatic treatments. They’re addressing the compensatory response (fast heart rate, low blood pressure) but not the root cause (poor venous return).
Our experience: “The medication keeps my heart rate from going as high, but I still feel awful when I stand.”
Exercise Reconditioning
Standard advice: Gradual exercise to recondition the autonomic nervous system.
Why it doesn’t fully work: If your venous return is structurally impaired, exercise can actually make things worse. You’re asking a compromised system to do more work.
Our experience: “Every time I try to exercise, I crash for days afterward.”
How to Know If Venous Compression Is Driving Your POTS
Red flag symptoms that suggest venous insufficiency:
- Left leg symptoms more than right
- Swelling, heaviness, discomfort primarily in left leg
- Visible varicose veins or spider veins on left leg
- Left leg feels “tired” or “heavy” by end of day
- Not a guarantee; some patients bilateral symptom burden is equal
- Pelvic symptoms
- Pelvic pain or pressure (especially in women)
- Pain that worsens with prolonged standing
- Relief when lying down with legs elevated
- Worse in the morning
- Visible bloating
- Skin changes
- Red or purplish-brown discoloration on legs
- Hemosiderin deposits (brownish staining from old blood)
- Visible venous pooling when standing
- Positional worsening
- POTS symptoms dramatically worse after standing/sitting for extended periods
- Significant improvement when legs are elevated
- “I feel best lying down with my feet up”
- Post-exertional crashes
- Walking, standing, or light activity triggers severe crashes
- Recovery takes days, not hours
- Exercise intolerance seems disproportionate to deconditioning
- Mast Cell Activation Symptoms
– Flushing episodes, especially in legs or pelvis, but can be systemic
– Hives or skin reactions that worsen with standing
– Abdominal pain, bloating, or digestive issues (pelvic venous congestion affecting GI tract with some experiencing IBS)
– Histamine intolerance symptoms that correlate with POTS flares
– “I have both POTS and MCAS and they seem to trigger each other” - Worsening MCAS with Venous Symptoms
– MCAS flares worsen in the morning (as venous pooling worsens overnight)
– Flushing and hives worse in the evenings
– Antihistamines help MCAS but don’t touch the POTS
– “My mast cell symptoms are worse when my legs are swollen”
We have even seen some patients developing autoimmune conditions of the CNS. After undergoing interventions for Iliac Venous Compression, these patients saw symptoms related to these conditions going into remission. This is a clinical observation, and more study is required to understand the link between venous compression, pelvic blood stasis, and CNS autoimmunity.
If you have several of these, venous compression should absolutely be evaluated.
Diagnostic Testing for Venous Compression
If we suspect venous compression based on symptoms, here’s how we evaluate:
Gold Standard: MRI Venography & MRI Angiography
- Detailed view of pelvic vasculature
- Visualizes the iliac veins and arteries, and extent of compression
- Can identify May-Thurner Syndrome, Nutcracker Syndrome, pelvic congestion
- Best non-invasive diagnostic tool
Based on our work with Dr. Brooke Spencer, and Interventional Radiologist with decades of experience treating Iliac Venous Compression, her specific MRV and MRA protocol that we use is the only way to identify Iliac Venous Compressions that do not involve a Deep Vein Thrombosis.
Most Definitive: Intravascular Ultrasound (IVUS)
- Performed during venography
- Provides detailed assessment from inside the vein
- Can measure exact degree of compression
- Often done if stenting is being considered
Our approach: We typically start with symptoms and clinical examination. If venous compression is suspected, we refer for appropriate imaging. The key is working with vascular specialists who understand the POTS connection, such as Dr. Brooke Spencer.
Treatment Approaches for Venous Compression in POTS
When we identify venous compression as a driver of POTS, we have several treatment options:
Conservative/Medical Management
For mild to moderate compression, we start with:
1. Flavay (Oligomeric Proanthocyanidins)
Supports vascular health and collagen integrity.
- Strengthens blood vessel walls
- Reduces inflammation
- Improves venous tone
- Supports endothelial function
Additional benefit for MCAS patients: Flavay (OPCs) also has mast cell stabilizing properties. By supporting vascular integrity AND stabilizing mast cells, it addresses both the venous compression and the MCAS component simultaneously.
Why it works for spike protein damage: Helps repair the collagen and endothelial dysfunction caused by spike. Think of it as rebuilding the structural integrity of your veins.
2. Sulodexide
A glycosaminoglycan that improves endothelial function and reduces venous insufficiency.
- Restores endothelial barrier function
- Reduces inflammation in vessel walls
- Improves blood flow
- Decades of use for chronic venous insufficiency in diabetic patients in the EU
Why this also matters for MCAS:
By restoring endothelial function and improving venous drainage, sulodexide reduces the hypoxic and inflammatory triggers that cause mast cell degranulation. Many patients report improvement in both POTS and MCAS symptoms.
Why it works for Long COVID/PVS: Directly addresses the endothelial dysfunction caused by spike protein. Fast-moving heparin penetrates the endothelium at a deeper level, reaching and healing the glycocalyx. Multiple studies show improvement in venous function.
Typical protocol: Usually combined with other interventions targeting spike protein clearance and vascular repair. Treatment duration varies. It is very important to note that the underlying spike protein pathology needs to be addressed. The endothelial impacts are systemic, and will cause other future conditions. However, Iliac Venous Compression is a significant and serious bottleneck deserving of immediate attention.
3. Softwave Therapy
Regenerative therapy that promotes tissue healing.
- Stimulates collagen production
- Improves blood flow
- Reduces inflammation
- Promotes vascular regeneration
Why it works: Helps rebuild the damaged connective tissue and vascular structures affected by spike protein. There are already sexual health clinics that have used Softwave Therapy for many years to help male patients with Erectile Dysfunction, indicating the efficacy of healing the vasculature.
Interventional Treatment: Venous Stenting
For moderate to severe compression that doesn’t respond adequately to conservative treatment:
What it is: Minimally invasive procedure where a balloon widens the compressed vein, then a stent is permanently placed to hold it open and restore normal blood flow.
When we consider it:
- Significant compression (>50%) on imaging
- Conservative treatment hasn’t provided adequate relief
- Symptoms are severely impacting quality of life
- Patient is motivated for intervention
Success rates: Research shows significant symptom improvement in POTS patients after iliac vein stenting:
- 83% of POTS patients** have confirmed venous compression on imaging (eClinicalMedicine, 2026)
- Significant quality of life improvements** at 3 and 12 months post-stenting, with improvements in physical functioning (+19 points), energy/fatigue (+13 points), pain (+10 points), and social function (+26 points) (JACC, 2024)
- 97.1% stent patency** at 3 years for non-thrombotic iliac vein compression (the type POTS patients have) – the best outcomes of all venous stenting groups (ABRE study, 2021)
- 90-95% long-term patency rates** across multiple large studies
- Low complication rates:** 1.7% major bleeding, 0% stent fractures in dedicated venous stents
At Leading Edge Clinic, our observations have mirrored what was found in these studies, with some caveats. Because Long Covid and Post-Vaccine Syndrome are complex, multi-system conditions, there is other intervention required for ongoing health. However, our patients nearly always see a significant improvement in POTS symptoms following appropriate intervention for Iliac Venous Compressions. We work with experts like Dr. Brooke Spencer because of her pioneering in the space. Stenting alone requires specialized knowledge of the condition (ie: appropriate stent size for patients).
Important caveat: This is typically done in conjunction with other Long COVID/PVS treatments. Venous compression is often one piece of a multi-system problem.
Why This Is Rarely Diagnosed
You might be wondering: If 50-70% of POTS patients have venous compression, why isn’t this being diagnosed more often?
Several reasons:
1. Most Doctors Aren’t Looking for It
Standard POTS evaluation focuses on:
- Tilt table test
- Autonomic testing
- Heart rate and blood pressure monitoring
Pelvic venous imaging isn’t part of the typical POTS work-up. Unless you’re seeing a vascular specialist, it often gets missed. “Standard of Care” for iliac venous compression is to only look for it, and only treat it if patients are positive for a Deep Vein Thrombosis in the affected area.
2. Symptoms Overlap
The symptoms of venous insufficiency (fatigue, dizziness, exercise intolerance) overlap completely with general POTS symptoms. Without specific venous symptoms (leg swelling, pelvic pain), doctors don’t think to check. Patients can have IVC without leg swelling and pelvic pain.
3. Vascular and Autonomic Specialists Don’t Often Communicate
POTS patients usually see cardiologists or autonomic specialists. Venous compression is diagnosed by vascular surgeons or interventional radiologists. These specialties don’t always talk to each other about the same patient. Furthermore (and to reiterate), many vascular surgeons have been trained to only look for, and intervene on Iliac Venous Compressions if patients develop a Deep Vein Thrombosis in the left common iliac vein.
4. It’s a Relatively New Connection
The research connecting POTS and venous compression has mostly emerged in the last 5-10 years. Many doctors simply aren’t aware of this link yet. Specialists like Dr. Brooke Spencer have been observing this clinically for over two decades, while many of her colleagues have followed standard of care that ignores this connection.
5. Long COVID and PVS Are Making It More Common
The spike protein-induced vascular damage is likely increasing the prevalence beyond what we saw in traditional POTS. We’re seeing this connection more and more in our Long Covid and Post-Vaccine Syndrome patients
Our Comprehensive Treatment Approach
At Leading Edge Clinic, we don’t just treat POTS symptoms. We look for and address the root causes, including venous compression.
Here’s our approach:
Step 1: Comprehensive Evaluation
- Detailed symptom history (looking for venous insufficiency clues)
- Physical examination
- Review of any previous imaging
- Assessment for other Long COVID/PVS mechanisms
Step 2: Root Cause Assessment
We evaluate for multiple mechanisms that can drive POTS in Long COVID/PVS:
- Venous compression and insufficiency
- Persistent spike protein
- Immune dysregulation (autoantibodies to adrenergic receptors)
- Mitochondrial dysfunction
- Autonomic nervous system dysfunction
- Microclot formation
- Mast cell activation (and how it interacts with venous compression)
- Our complete treatment framework addresses 7 root cause of Long Covid and Post-Vaccine Syndrome
POTS is rarely one thing. It’s usually multiple dysfunctions working together.
Step 3: Multi-Targeted Treatment
If venous compression is present:
- Start with vascular support (Flavay, Sulodexide)
- Consider Softwave therapy
- Refer to interventional radiology or vascular specialist if imaging shows significant compression
- Coordinate care if stenting is pursued
Simultaneously address:
- Spike protein clearance
- Endothelial repair
- Immune modulation (if autoantibodies present)
- Mitochondrial support
- Autonomic retraining
- Mast cell stabilization (especially important if venous compression is triggering MCAS)
Plus conventional POTS support:
- Salt and hydration (still helpful even if not the primary solution)
- Compression (can help lower leg pooling)
- Medication if needed for symptom control
- Gradual reconditioning when ready
Step 4: Monitor and Adjust
- Regular follow-ups to assess response
- Adjust treatment based on symptom improvement
- Coordinate with vascular specialists as needed
- Continue addressing underlying Long COVID/PVS mechanisms
What to Expect: Recovery Timeline
If venous compression is a major driver and you get appropriate treatment:
Weeks 1-4 (Conservative Treatment)
- Start vascular support interventions
- May notice reduction in leg heaviness
- POTS symptoms still present but potentially less severe
Weeks 4-12
- If Flavay/Sulodexide are helping, progressive improvement in venous symptoms
- POTS may start improving as venous return improves
- Can often begin gentle reconditioning
Months 3-6
- Continued improvement in both venous and POTS symptoms
- Many patients report being able to tolerate upright posture longer
- Exercise tolerance often improves
- Some patients ready for interventional options if conservative treatment plateaus
If Stenting Is Performed
- Immediate restoration of venous flow
- Many patients report rapid improvement in POTS symptoms (within days to weeks), with some improvements taking longer (months)
- Continued improvement over months as other mechanisms are addressed
- Not a cure-all (you still need to address spike protein, immune issues, etc.), but can be dramatically helpful for the venous component
Key point: If venous compression is your primary POTS driver and it gets treated effectively, improvement can be substantial. But if there are multiple mechanisms (which is common), you need a comprehensive approach.
Clinical Insights from 3,500+ Patients
What predicts treatment success?
Based on our clinical experience, patients who respond best to venous compression treatment share these characteristics:
✓ Younger age (under 50) – better vascular remodeling capacity; though this does not mean patients above 50 do not see significant improvement
✓ Shorter duration of symptoms (under 2 years) – less unchecked vessel damage; again, does not indicate significant improvement is unlikely
✓ Higher baseline function (can stand 10+ minutes) – indicates some compensatory mechanisms intact
✓ Positive response to trial interventions (sulodexide, Flavay) within 4-6 weeks
What makes treatment more challenging?
⚠ Long symptom duration (3+ years) – more fibrotic vessel changes
⚠ Severe autonomic dysfunction (can’t stand at all) – multiple mechanisms involved
⚠ Significant comorbidities (MCAS, EDS, autoimmune) – complexity requires longer treatment
⚠ Ongoing spike protein exposure (repeat infections, ongoing vaccination)
The bottom line:
Early intervention yields best results. Waiting 2-3 years while trying ineffective treatments allows more permanent vascular damage.
Why This Matters for Long COVID and Post-Vaccine Syndrome
Standard POTS treatment was developed for idiopathic POTS (POTS without a clear cause).
But Long COVID and Post-Vaccine Syndrome POTS is different. It has specific mechanisms:
- Spike protein-induced endothelial damage
- Collagen dysfunction
- Immune dysregulation
- Persistent inflammation
These mechanisms aggressively contribute to venous compression and insufficiency.
This is why generic POTS protocols often fail in Long COVID/PVS patients.
You can’t treat Long COVID POTS the same way you treat traditional POTS. You have to address the spike protein damage, the vascular dysfunction, the immune issues—all of it.
And if you don’t evaluate for and treat venous compression when it’s present, you’re missing a massive piece of the puzzle in 70%+ of patients.
The POTS-MCAS Connection in Long COVID and Post-Vaccine Syndrome
One of the most common patterns we see in Long COVID and Post-Vaccine Syndrome patients:
They develop POTS and MCAS together. This isn’t a coincidence. Here’s why:
Spike Protein Creates the Perfect Storm
Spike protein damages multiple systems simultaneously:
1. Endothelial dysfunction → venous compression, poor vascular function
2. Immune dysregulation → mast cell activation, histamine intolerance
3. Collagen dysfunction → weakened veins (more compression), tissue fragility
The result?
- Venous compression drives POTS
- Venous congestion triggers MCAS
- MCAS worsens vascular inflammation
- Worse inflammation → more venous dysfunction
- Self-perpetuating cycle
Why Treating Just One Condition Fails
If you only treat MCAS:
- Antihistamines, mast cell stabilizers, low-histamine diet
- Helps temporarily, but venous compression keeps triggering mast cells
- MCAS symptoms return or plateau
If you only treat POTS:
- Salt, compression, beta-blockers
- Helps some symptoms, but doesn’t address mast cell inflammation
- MCAS continues driving vascular dysfunction
If you treat venous compression as part of comprehensive care:
- Address structural problem (venous obstruction)
- Reduce mast cell triggers (hypoxia, congestion)
- Support vascular healing (Flavay, Sulodexide)
- Stabilize mast cells simultaneously
- Both conditions improve together
This is why our approach addresses all mechanisms simultaneously. You can’t separate POTS from MCAS from venous compression in Long COVID and Post-Vaccine Syndrome patients. They’re interconnected parts of the same spike-driven pathology.
Red Flags You’re Not Getting Proper POTS Care
Be wary if your doctor:
🚩 Never asks about leg symptoms (swelling, heaviness, varicose veins)
🚩 Doesn’t consider venous imaging when standard treatments aren’t working
🚩 Treats your POTS exactly like every other POTS patient (cookie-cutter approach)
🚩 Doesn’t acknowledge the spike protein connection in Long COVID/PVS POTS
🚩 Only offers salt, fluids, and compression stockings without investigating why these aren’t working
🚩 Dismisses your symptoms as “just anxiety” or “deconditioning”
🚩 Doesn’t coordinate with vascular specialists when venous issues are suspected
🚩 Treats POTS and MCAS as separate conditions (doesn’t understand they’re often mechanistically linked)
🚩 Ignores the venous compression-MCAS connection (keeps adding MCAS medications without investigating why mast cells keep degranulating)
What good POTS care looks like:
✓ Comprehensive evaluation including vascular symptoms ✓ Considers multiple mechanisms (not just autonomic dysfunction) ✓ Refers for appropriate imaging when venous compression is suspected ✓ Coordinates care between specialties (interventional radiology, etc…) ✓ Addresses the specific mechanisms of Long COVID/PVS POTS ✓ Combines conventional POTS support with root cause treatment ✓ Regular monitoring and adjustment based on response ✓ Understands the POTS-MCAS connection in Long COVID/PVS ✓ Evaluates for venous compression in patients with treatment-resistant MCAS ✓ Treats the underlying triggers (venous congestion, hypoxia) not just MCAS symptoms
The Bottom Line
If POTS is a significant symptom of your Long Covid or Post-Vaccine Syndrome presentation and standard treatments aren’t working, there’s a very real possibility that venous compression is part of your problem.
This isn’t rare. Research shows 50-70% of POTS patients have significant venous insufficiency. And spike protein damage makes it even more common in Long COVID and Post-Vaccine Syndrome patients.
The good news? When venous compression is identified and treated appropriately, many patients see substantial improvement.
The bad news? Most doctors aren’t checking for this. You may need to advocate for yourself to get proper evaluation.
Next Steps
If you recognize yourself in this article:
If You Haven’t Been Evaluated for Venous Compression
- Document your symptoms – especially left leg heaviness, pelvic symptoms, positional worsening
- Request vascular imaging – ensure the MRV and MRA follow the Spencer protocol
- Find doctors who understand this connection – specialists familiar with POTS, or Long COVID/PVS specialists who coordinate with experts in interventional readiology or vascular care
If You Need Specialized Care
At Leading Edge Clinic, we’ve treated thousands of Long COVID and Post-Vaccine Syndrome patients with POTS. We:
- Routinely evaluate for venous compression in our POTS patients
- Offer comprehensive treatment addressing all mechanisms (including vascular dysfunction)
- Coordinate with vascular specialists when stenting or other interventions are needed
- Provide nationwide telehealth (all 50 states)
Ready to get started?
- Register as a patient – Nationwide telehealth available in all 50 states
- Learn about our treatment approach
- Access patient success stories
- Our Expertise
Still learning?
- Long COVID vs Post-Vaccine Syndrome: What’s the Difference?
- 7 Warning Signs You Have Post-Vaccine Syndrome
- Browse all Long COVID and PVS resources
A Final Word
You’ve probably been told your POTS symptoms are “just” autonomic dysfunction. That you need to drink more water, add more salt, exercise more.
But if there’s a compressed vein blocking blood return to your heart, all the salt in the world won’t fix that.
You’re not failing at POTS treatment. The standard approach is failing to identify what’s actually wrong.
Venous compression is real. It’s measurable. It’s treatable.
And when it’s the primary driver of your POTS, addressing it can be life-changing.
You deserve doctors who look for the actual cause, not just treat the symptoms.
You deserve comprehensive evaluation.
And you deserve treatment that works.
Additional Clinical Resources
For deeper dives into specific cases and treatment protocols, Scott Marsland FNP-C (practice partner at Leading Edge Clinic) shares detailed clinical observations on his Substack:
Case Studies:
– Iliac Venous Compression Case Study – Detailed workup and treatment approach
– Clinical Observations on Venous Insufficiency – Pattern recognition in practice
– Sulodexide Protocol and Outcomes – In-depth treatment guide
These articles provide the level of clinical detail typically reserved for medical conferences and peer discussions. However, they are not intended as medical advice. Please consult with a qualified medical professional.
References:
Primary POTS-Venos Compression Studies
1. Spencer EB, Saikia J, Ajeya D, Phillips R, Cutchins A, et al. Association and post-iliac vein stenting symptom improvement of postural orthostatic tachycardia syndrome and orthostatic intolerance with pelvic venous disorders: two retrospective studies. eClinicalMedicine. 2026. https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(26)00019-2/fulltext
2. Iliac vein stenting and quality of life in patients with postural orthostatic tachycardia syndrome (POTS). Journal of the American College of Cardiology. 2024. https://www.jacc.org/doi/10.1016/S0735-1097(24)04303-1
3. Brown MT, Pelling MM, Cutchins A, Gilliland CA. Left common iliac vein stenting in a case of postural orthostatic tachycardia syndrome/pelvic pain overlap. Cureus. 2024;16(3):e55974. https://pmc.ncbi.nlm.nih.gov/articles/PMC10927248/
4. Knuttinen MG, Naidu SG, Oklu R, Kriegshauser S, Eversman W, Rotellini L, et al. Imaging findings of pelvic venous insufficiency in patients with postural orthostatic tachycardia syndrome. Clinical Imaging. 2020;64:83-87. https://pubmed.ncbi.nlm.nih.gov/32757696/
5. Ormiston CK, Qadri SK, Gurram N, Singh I, Siddiqui AH. May-Thurner syndrome in patients with postural orthostatic tachycardia syndrome and Ehlers-Danlos syndrome: a case series. European Heart Journal – Case Reports. 2022;6(4):ytac161. https://academic.oup.com/ehjcr/article/6/4/ytac161/6565741
6. Pelvic vein compression in patients diagnosed with postural orthostatic tachycardia syndrome. Circulation. 2023;148(Suppl_1):Abstract 15621. https://www.ahajournals.org/doi/10.1161/circ.148.suppl_1.15621
7. Spencer EB, Saikia J, Ajeya D, Phillips R, Cutchins A. Symptomatic improvement in orthostatic intolerance and postural orthostatic tachycardia syndrome and pelvic pain after iliac vein stenting. SSRN. 2025. https://papers.ssrn.com/sol3/papers.cfm?abstract_id=5235054
General Venous Stenting Outcomes
8. A meta-analysis of the medium- to long-term outcomes in patients with chronic deep venous disease treated with dedicated venous stents. Journal of Vascular Surgery: Venous and Lymphatic Disorders. 2023. https://www.sciencedirect.com/science/article/pii/S2213333X23004389
9. Final 3-year study outcomes from the evaluation of the Zilver Vena venous stent for the treatment of symptomatic iliofemoral venous outflow obstruction (The VIVO Clinical Study). Journal of Vascular and Interventional Radiology. 2024. https://www.jvir.org/article/S1051-0443(24)00209-4/fulltext
10. 36-month outcomes of the ABRE study evaluating the safety and effectiveness of the Abre venous self-expanding stent system. Journal of Vascular and Interventional Radiology. 2021. https://www.sciencedirect.com/science/article/abs/pii/S2213333X21000688
11. Razavi MK, Jaff MR, Miller LE. Safety and effectiveness of stent placement for iliofemoral venous outflow obstruction: systematic review and meta-analysis. Circulation: Cardiovascular Interventions. 2015;8(10):e002772. https://www.ahajournals.org/doi/10.1161/circinterventions.115.002772
12. Ikezawa T, Naiki M, Nakamura M, Ishii H, Kumada Y, Ogino H. Venous stenting for postthrombotic iliocaval venous obstructive disease: clinical efficacy and mid-term outcomes. Annals of Vascular Diseases. 2021;14(2):99-105. https://pmc.ncbi.nlm.nih.gov/articles/PMC9816030/
13. Clinical outcomes at 3 years after stenting for thrombotic and non-thrombotic iliac vein compression syndrome patients. Journal of Interventional Medicine. 2024;7(1):30-38. https://pmc.ncbi.nlm.nih.gov/articles/PMC10787525/
14. Outcomes following iliac vein stenting for non-thrombotic iliac vein lesions—a narrative review based on large sample studies. Life. 2025;16(12):427. https://www.mdpi.com/2079-4983/16/12/427
15. A comprehensive study on venous endovascular management and stenting in deep veins occlusion and stenosis: a review study. Cardiovascular Revascularization Medicine. 2024. https://www.sciencedirect.com/science/article/pii/S2589845024000526
16. Quality of life outcomes for patients undergoing venous stenting for chronic deep venous disease. Journal of Vascular Surgery: Venous and Lymphatic Disorders. 2021. https://www.sciencedirect.com/science/article/abs/pii/S2213333X21000688
17. Raju S, Neglén P. Iliac vein compression: epidemiology, diagnosis and treatment. Annals of Vascular Diseases. 2019;12(2):169-181. https://pubmed.ncbi.nlm.nih.gov/31190849/
POTS-Venous Disease Connection
18. McDermott M. Mast cell masterminds #1: the pelvic venous syndromes and ME/CFS, POTS, and long COVID. Health Rising. 2025. https://www.healthrising.org/blog/2025/09/24/pelvic-venous-syndromes-pots-chronic-fatigue-long-covid/
19. Is May-Thurner syndrome linked to Ehlers-Danlos syndrome and POTS? The EDS Clinic. 2025. https://www.eds.clinic/articles/may-thurner-syndrome-ehlers-danlos-syndrome-pots
20. Connecting heart conditions: POTS, MTS, PCS & EDS. CardioVascular Health Clinic. 2025. https://cvhealthclinic.com/news/pots-mts-pcs-eds-treatment-oklahoma/
Orthostatic Symptoms and Venous Stenting
21. Iliac venous stenting as adjunct in the management of symptomatic orthostatic hypotension in iliac vein compression. Journal of Vascular Surgery Cases, Innovations and Techniques. 2024;10(2):101674. https://www.sciencedirect.com/science/article/pii/S2468428724000674
22. Venous clinical severity score has a suboptimal ability to detect improvement after iliac vein stenting across three years of follow-up. Journal of Vascular Surgery: Venous and Lymphatic Disorders. 2023;11(4):829-838. https://pubmed.ncbi.nlm.nih.gov/36906105/
This article is for informational purposes only and does not constitute medical advice. POTS evaluation and treatment should be undertaken with qualified medical supervision.
About Leading Edge Clinic
We specialize in treating Long COVID, Post-Vaccine Syndrome, POTS, MCAS, and related conditions. Since 2020, we’ve treated thousands of patients nationwide via telehealth, with a focus on identifying and addressing root causes rather than just managing symptoms.
Learn more: drpierrekory.com